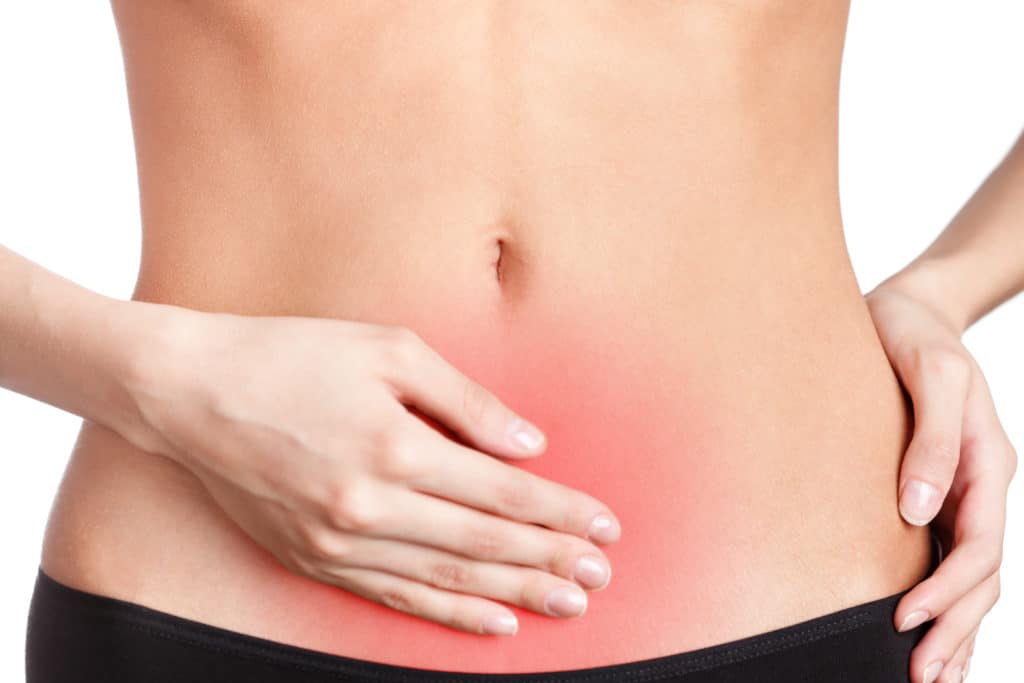
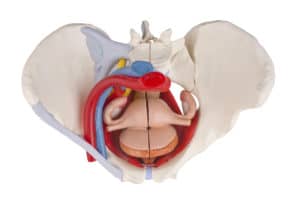
Are you a female with pain below your belly button?
If the pain is in your lower abdomen area, where we usually feel menstrual cramps, childbirth contractions or ovulation pain, it could be pelvic pain.
If so, you’re not alone. Many women feel pain in their lower abdomen at various points in their lives, often for no apparent reason.
At Nancy Branberg PT, we understand that pelvic pain negatively affects your sex life, sleep, sense of wellbeing, and your ability to exercise and enjoy life. It can be debilitating.
But it doesn’t have to be that way.
Sometimes it’s a pain that occurs during intercourse – which we call “Dyspareunia”, pain during your annual gynecology exam ,or pain while using tampons. For some women, gynecology exams and using tampons become impossible.
Other times it a chronic dull ache that never seems to go away, in extreme cases, for decades. It’s very common. Yet, the problem is well-meaning friends and relatives lead us to believe it’s normal, particularly after having children or getting older. It isn’t, and you don’t have to put up with it.
We’re experts in women’s health. Our mission is to provide the answers to all the questions you’re too embarrassed to ask. We can help you understand what happens in the bathroom and the bedroom.
This blog explains what pelvic pain is, what causes it, and how to treat it.
Don’t suffer in silence. Life is short. Read on to get help now.
What Causes Pelvic Pain?
Well, as you can probably imagine – due to the number of different organs and delicate structures inside the female pelvis – there is no one cause of pelvic pain.
Each case and each woman is different. Men suffer from pelvic pain, too, of course – from inflammation of the prostate, bowel problems, and urinary tract infections, but on a much less regular basis than women due to menstruation, childbirth, and other female-only biological processes. So, it’s a much more common problem in women.
Sometimes, the issue is not physical at all, and it’s psychological in nature. Nevertheless, we feel it as physical pain due to stress-related tension in your muscles, fascia, and connective tissue.
This muscle tension may be the case for you, or it may be something different altogether, causing your internal pain. With this in mind (if you haven’t done so already), we recommend a consultation with your doctor.
This consultation is so your doctor can rule out any apparent cause of your pelvic pain, such as a bacterial infection, ovarian cyst, uterine fibroids, or any other issue that requires immediate medical attention. But if it transpires – as is the case with lots of women – there is no apparent cause for your discomfort.
Let’s examine some of the other possible causes of pelvic pain:
Nerve Irritation
Nerve irritation is one of the many causes of pelvic pain overlooked by MDs, simply because it’s not visible on imaging tests.
There is a major nerve that runs from the base of your vagina to your pelvic floor muscles. This vital nerve controls your sphincter muscles, too. There is a condition called Pudendal Nerve Neuralgia that involves this nerve and causes pelvic pain.
Still, it is much more likely to be sharp, shooting pain associated with nerve-related pain. It may also present with muscle weakness or pins and needles. However, there is a spider’s web of nerves in your pelvic area, and it could be any of one of the thousands that are causing your symptoms. A Physical Therapist can diagnose whether nerve irritation is the cause of your pelvic pain.
Interstitial Cystitis
Unlike regular cystitis, interstitial cystitis isn’t caused by bacteria or a so-called “bladder infection”. The symptoms differ from the burning pain of normal cystitis. Instead, interstitial cystitis causes chronic pelvic pain, a strong urge to urinate – that causes you to need to urinate more regularly, most-notably multiple times during the night.
It’s sometimes referred to as “painful bladder syndrome,” too. So, if this type of cystitis is the cause of your pelvic pain, you’re more likely to feel it around your bladder (although not exclusively).
Chronic Constipation
The critical thing to remember about constipation, especially when it’s chronic, is that you may still have a regular bowel movement and not notice any symptoms. However, your lower colon is still partially impacted.
This problem is one of the most common reasons we see pelvic pain in the clinic. If you’re constipated, it has a knock-on effect on the organs, muscles, and nerves in your lower abdomen, which leads to pelvic pain.
If you’re stressed, you may have “functional constipation”. This condition is when you tense your body and sphincter muscles so much that you prevent your body from having a bowel movement.
Pelvic Floor Dysfunction
Pelvic floor dysfunction is the overarching reason why women experience pelvic pain when there is no apparent cause. Even in the case of interstitial cystitis, constipation, and nerve pain, it’s the stiffening and tightening of the pelvic floor and the pelvic floor muscles that causes long-term, chronic pain. And the key to treatment, once we find the cause, is to strengthen and relax the pelvic floor muscles.
Like the muscles in the rest of your body, the pelvic floor muscles can lose strength, tighten, tear and become weak. Age and childbirth can exacerbate this process, but it’s not something you have to endure.
Your Physical Therapist can find and treat the root cause and give you exercises to overcome the specific pelvic floor problems you’re experiencing.
How to Treat Pelvic Pain
You won’t be surprised to hear that the most effective way to treat chronic pelvic pain is to book an appointment with a Physical Therapist. We offer all new patients a complimentary call with one of our Physical Therapists. This way, we can discuss your symptoms, ask questions, and determine whether Pelvic Physical Therapy is right for you. We also offer a free, 30-minute taster session at our clinic in Falls Church, VA. Choose whichever works best for you.
In the meantime, there are some things you can do to ease your pelvic pain symptoms immediately. Here are some of our favorites:
Walk
With severe pelvic pain, regular exercise forms may be difficult, but taking a walk outdoors works wonders for chronic pain symptoms. It gets your blood flowing – pumping oxygen to your pelvic area. It also reduces pain and eases the symptoms of anxiety and depression that often accompany chronic pain.
Stay Hydrated
One of your body’s many cries for water is pain. When you’re dehydrated, everything feels worse. Keep your pain symptoms in check and reduce your reliance on painkillers by staying hydrated throughout the day. If you don’t like plain water, try adding a squeeze of fresh lemon or lime or drink fruit tisanes and herbal tea. If you’ve been working out or the weather is really hot, remember to drink extra to replenish lost fluids due to sweating.
Limit Sitting
It might be tempting, especially when you’re in pain, to rest as much as possible. In this case, however, the worst thing you can do for pelvic pain is sitting back on your tailbone for long periods. Sitting for longer than half an hour causes your muscles to tighten and stiffen, which can worsen the pain. Set a timer and make a conscious effort to get up from your desk or couch and take a walk around the room.
Eat Well
As the saying goes, you are what you eat. If you give your body good food – with lots of vitamins, minerals, and nutrients, your body is more able to heal and repair. Processed foods with excess sugar and salt have been proven to make pain symptoms worse, so avoid where possible. Choose fresh fruit and vegetables between meals instead of reaching for sugary snacks and chips.
You might also want to consider keeping a food diary to track whether there are any foods, or combinations of foods, that make your symptoms worse.
How do you react to caffeine? Sugar? Dairy? Alcohol?
Breathe
The breath is a potent mediator of your nervous system. Fast, shallow breathing activates your sympathetic nervous system and the fight or flight response, making you feel more stressed and tense. You’re ready to fight. Conversely, long, deep breaths slow the heart rate and activate the sympathetic nervous system and the stretch and relax response.
When your body is in a relaxed state, pain symptoms reduce – particularly in pelvic pain. Try to include a relaxing “breath practice” into your daily routine.
Talk To A Physical Therapist About Your Pelvic Pain
Are you ready to solve your pelvic pain problems?
Contact us now to book your complimentary call or Discovery Visit to see if we are a good fit for you. We’re passionate about helping women embarrassed by incontinence. Are you a women struggling with pelvic pain, dealing with digestive issues, or wanting to feel confident and fit after baby (even if it’s been 30 years)? We’re here to help you.
Shift your energy and attention to all the things you love to do.